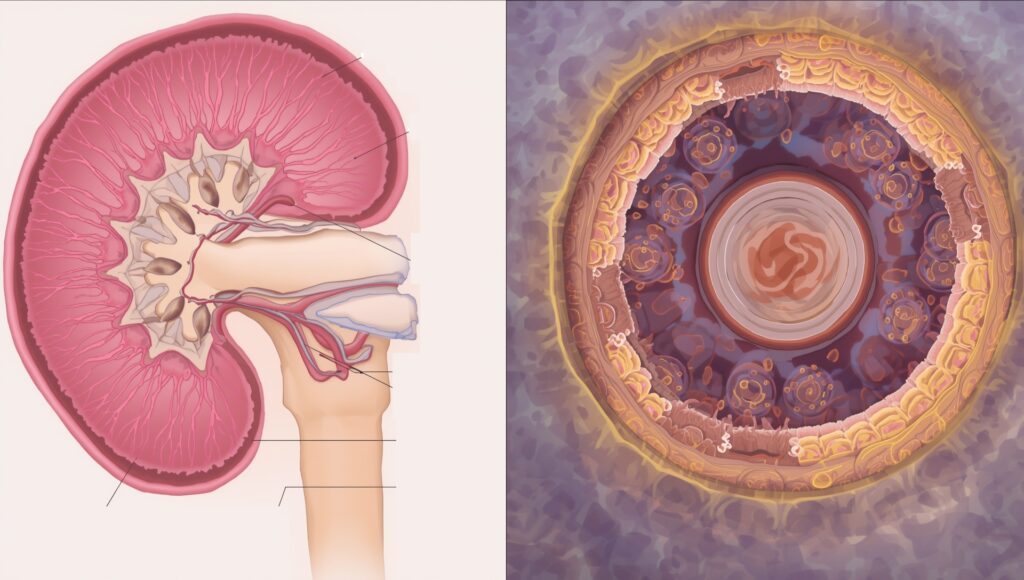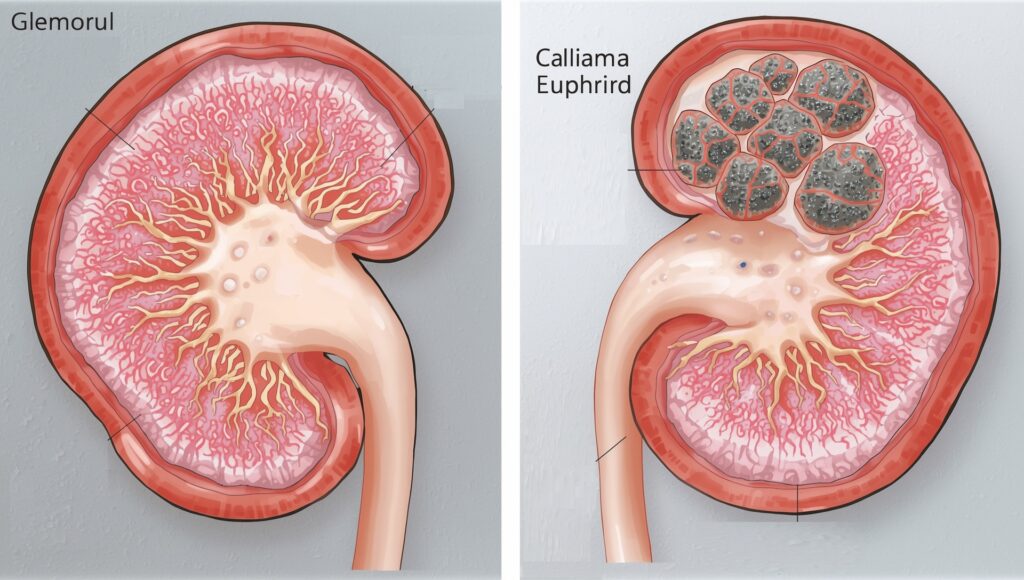
Etiology of Renal Failure and its importance to Introduction
Renal failure, or kidney failure, is a leading medical emergency that makes your body unable to carry out waste and remove consummate liquid from the decayed blood. It’s important to know the fundamentals about kidney failure because the kidneys keep you alive. If these organs are not working as they should, dangerous toxins may build up with the potential to cause serious complications.
Renal failure can generally be categorized into two primary types: Acute Renal Failure, which is a sudden loss of kidney function; and Chronic Renal Failure. Both types can profoundly affect an individual’s quality of life and prompt early medical attention is essential.
Naturally, the health of your kidneys is vital. At least two healthy kidneys are known to control blood pressure, balance electrolytes and promote red blood cells. Knowing about Renal failure and and its Early kidney-failure warning signs —including swelling, fatigue, or changes in urination — may help lead to early diagnosis and better treatment.
With knowledge on kidney failure basics, as well as maintaining one’s kidney health for check-ups and healthy living can keep these serious issues far away.
Etiology of Renal Failure Comparison of Acute vs. Chronic
Knowing the two main types of kidney failure – Acute and Chronic – is important for clinics and their patients. The causes for renal failure are types of Renal failure is generally categorized according to factors affecting the kidney function, which may be due to the duration and/or etiology.
Acute renal failure, or acute kidney injury (AKI), is an abrupt and usually reversible decline in the GFR. Causes of acute renal failure Working out what has caused your kidney damage helps doctors to treat the problem effectively. The most frequent causes are severe dehydration, blood loss, some infections, certain drugs and blockage in the urinary tract. As it comes on very fast, and if the underlying reason is treated right away, normal kidney function can usually be reestablished in time.
By contrast, Chronic Kidney Disease (CKD) progresses slowly and may take months or years of progression that is often irreversible. Etiological factors of the CKD are usually chronic with causes like diabetes, hypertension, chronic glomerulonephritis and long standing exposure to nephrotoxic drugs. These can all gradually cause the kidneys to no longer work as well.
The distinguishing features of acute and chronic renal failure are onset, reversibility, and causation. Acute renal failure tends to be a relatively fast and reversible condition which may require hospitalization, while chronic kidney disease is usually slow with irreversible loss of function. Understanding these differences is important for correct diagnosis, successful treatment, and better patient outcomes.
Pre-renal causes: reasons for reduced perfusion of the Kidneys
Pre-renal causes are the most frequent acute etiology of renal failure, and they develop as a result of decreased perfusion to the kidneys without actual damage to the renal tissue. Reduced renal perfusion can be very deleterious for the ability of kidneys to excrete waste and regulate fluid and electrolyte balance.
Hypovolemia is one of the most important pre-renal causes of renal failure. Hypovolemia means the volume of blood in a person is too low, and sometimes leads to the loss of body fluids, hemorrhaging and dehydration. In hypovolemia, there is not enough pressure to perfuse the kidneys properly and GFR decreases.
Also, heart failure is another important cause of impaired renal blood flow. Cardiac output decreases and renal perfusion decreases when the heart is not pumping well. This results in inadequate oxygenation of the kidney; this can progress to system level shutdown, and if not treated can lead to pre-renal azotemia very rapidly.
Other causes, such as severe burns, sepsis, and some drugs that affect blood pressure or vascular tone can also decrease renal perfusion. Identifying these pre-renal causes early is very important, since intervention (returning to normal state volume status or restoring heart function towards the baseline) may often result in a reversal of kidney injury before becoming irreversible.
Intrinsic (Renal) -Direct Trauma to the Kidneys
Intrinsic Renal Failure or Intrarenal failure results when the structures inside the kidneys are damaged causing them to be dysfunctional. Some of the more frequent causes of intrinsic renal failure are glomerulonephritis and acute tubular necrosis. Glomerulonephritis is often caused by an immune-mediated inflammation of the glomeruli, which can be triggered by infections, systemic diseases (such as lupus), or may result from an autoimmune disease. This inflammation destroys the filtering units in the kidneys, leading to a buildup of waste in the blood.
Another common cause is acute tubular necrosis (ATN), in which the tubule cells of the kidneys are injured. Causes of acute tubular necrosis include prolonged low blood flow (ischemia) and exposure to substances that are toxic to the kidneys. Certain drugs that are toxic to the kidneys (nephrotoxic)—such as antibiotics, nonsteroidal anti-inflammatory drugs (NSAIDs), and contrast agents used during imaging tests—damaging renal tubules (the microscopic parts of the kidney where urine is collected) can cause AKI.
Understanding these characteristic etiologies are so important for early intervention and avoiding additional insult to the kidneys. The prevention of renal damage requires early diagnosis and treatment of glomerulonephritis and acute tubular necrosis, as well as careful observation of nephrotoxic drug administration.
Post-Renal Causes: Urinary Outflow Tract Obstruction
Postrenal causes of renal failure Interrupted urine flow following the kidneys is blocked there. This blockage of the urinary passage out can produce pressure on the kidneys, causing them to work less and develop renal insufficiency and failure if not relieved promptly.
Kidney stone is regarded as one of the most predominant causes of urinary tract obstruction. They are hard mineral deposits that can develop anywhere in the urinary tract, making it impossible for urine to pass and causing a great deal of pain, as well as potential kidney damage. Prostatic hypertrophy of the prostate in elderly males is also a common post-renal cause of renal failure. A swollen prostate can squeeze the urethra, making urination a challenge as urine moves from your bladder through your penis—a compaction which can cause backup into kidneys and issues there later in time.
Strictures (narrowing) of the urethra, tumors that form in the urinary system, or pressure on it by a structure outside the urinary tract can all block urine flow. Identification and management of these post-renal causes are critical to prevent permanent renal damage and maintain urinary tract health.
Etiology of Renal Failure’ Standard Risk Factors
Prevention of progression of kidney disease to renal failure necessitates identifying the risk factors. Diabetes and hypertension are two of the largest contributors. The 2 are among the most common causes of chronic kidney disease (CKD) globally. Over time, diabetes can deteriorate the blood vessels in the kidneys and impair their ability to filter waste. So too does high blood pressure place additional strain on the kidneys’ fragile filtering system, thereby increasing risk for long-term injury.
Another important risk factor is having an inherited disposition to kidney diseases. People whose relatives have suffered from kidney diseases are more susceptible to such diseases themselves. Genetics can affect how the kidneys work, and genetics play a role in what happens when there are other medical problems at hand — which is why regular check-ups are even more critical for those who carry hereditary risk factors.
Obesity, smoking and some autoimmune disorders are among other things that can also play into the development and course of kidney disease. Knowing these factors you can make proactive choices, such as controling blood sugars and blood pressure, to have a healthier kidneys and reduce the chance of developing kidney disease.This -in turn- reduces your risk.
Infections and Autoimmune Pathogenesis of Renal Failure
Doreen January 23, 2014 Diseases Other than HIV Transplant & Donation Kidneys Urology Renal failure–the inability of the kidneys to function–can be caused by a multitude of underlying conditions, and infections as well as autoimmune diseases are among those that contribute. Infections that damage the kidneys are a big worry because some such bacteria, viruses and other germs can directly attack the kidney tissue.
For instance, if UTIs travel upward to the kidney, it can cause pyelonephritis: a serious infection that may scar the kidneys and result in chronic impairment of renal function. Furthermore, infectious diseases of the kidneys, like hepatitis B virus (HBV), hepatitis C virus (HCV) and HIV have been recognized to produce chronic inflammation and gradual renal damage.
Autoimmune Maladies Another major reason for R.F. prevalent is autoimmune disorder. In that context, the immune system erroneously attacks the body’s own tissues, including the kidneys. Autoimmune nephritis leads to kidney failure as a result of ongoing inflammation and scarring in the kidney’s filtering units (glomeruli). Lupus nephritis secondary to systemic lupus erythematosus (SLE) is one of the best recognized illustrations. In lupus nephritis, immune deposits form in the kidneys, triggering inflammation that can progress to chronic kidney disease and end-stage renal failure if not managed.
Insight into the pathogenesis of both infections and autoimmunity toward the kidney are necessary to make early diagnosis, designing appropriate treatments that prevent from renal failure progression.
Lifestyle and Environmental Risk Factors for Renal Injury
Mechanisms that cause damage to the kidneys must be better understood for both prevention and treatment of kidney disease. Bleak lifestyle factors some of the most markedly bleak lifestyle risk indicators are poor diet, sedentary living and chronic lack of hydration. High sodium diets, processed foods and overly acidic or protein-rich diet can compromise your kidneys ability to filter waste products. On the other hand low intake of fruits and veggies might make it harder for your body to fend off kidney injury.
Drug-related nephropathy should also be taken into account. Some drugs (such as some used in chemotherapy) can damage the kidneys directly, especially when taken over a long period of time. Other drugs have been reported to cause how to get weed out of your system naturally acute interstitial nephritis. People should use prescription and non-prescription drugs prudently and under the guidance of a healthcare provider to reduce their risk of renal injury.
Environmental nephrotoxins are also an emerging concern. “Exposure to heavy metals (lead, mercury, cadmium), industrial chemicals and pesticides could build up in the body and damage neutrons over time leading to chronic renal damage,” he said. Knowledge of such environmental threats and interventions to limit exposure are necessary measures in the protection of kidney health.
In the end, it’s a matter of eating a healthy diet, staying active, treating disease responsibly and avoiding harmful substances that pose an unnecessary burden on our environment — all in order to reduce your risk of kidney disease and protecting those kidneys for the long haul.
Prevention and Risk: Prevention Strategies Informed by Etiology
Renal failure can be avoided by knowing its etiology and applying specific measures. It is important to identify at-risk individuals early; regular screening for kidney function in certain groups (such as those with a family history or pre-existing conditions) provides the opportunity for early intervention. Among the key prevention measures, controlling hypertension and diabetes effectively are some of the most important, as uncontrolled blood pressure and blood sugar remain top causes for kidney damage. Through a combination of routine monitoring, medication compliance and close partnership with healthcare providers, these conditions can be controlled.
Healthy living is just as important as taking care of the kidneys. Eating a healthy diet low in salt and processed foods, keeping well-hydrated, exercising regularly and not smoking can also help to reduce the burden on the kidneys. With the combination of early detection, preventive management of comorbidities, and a positive lifestyle, people can reduce their risk of developing renal failure and maintaining kidney health in the long term.
Conclusions: Understanding the Origins/ Etiology of Renal Failure, to Improve Therapies
An insight into all causes of renal failure should help to improve patient care and ESRD prevention. Every underlying etiology — be it diabetes, hypertension, autoimmune diseases or inherited conditions — needs an individual specific pathophysiological approach. With proper cause determination, treatment and management plans can be directed, thus delaying progression of the disease. There is also a need to intervene in the early stage in cases of risk factors, such as high blood pressure, hyperglycemia and exposure to nephrotoxic agents.
Early detection and education give patients the knowledge to make informed lifestyle changes which will ultimately decrease the occurrence of, or the severity of renal failure. By focusing on prevention as well as personalised care, I believe we can make huge inroads into tackling this very complicated and difficult disease.